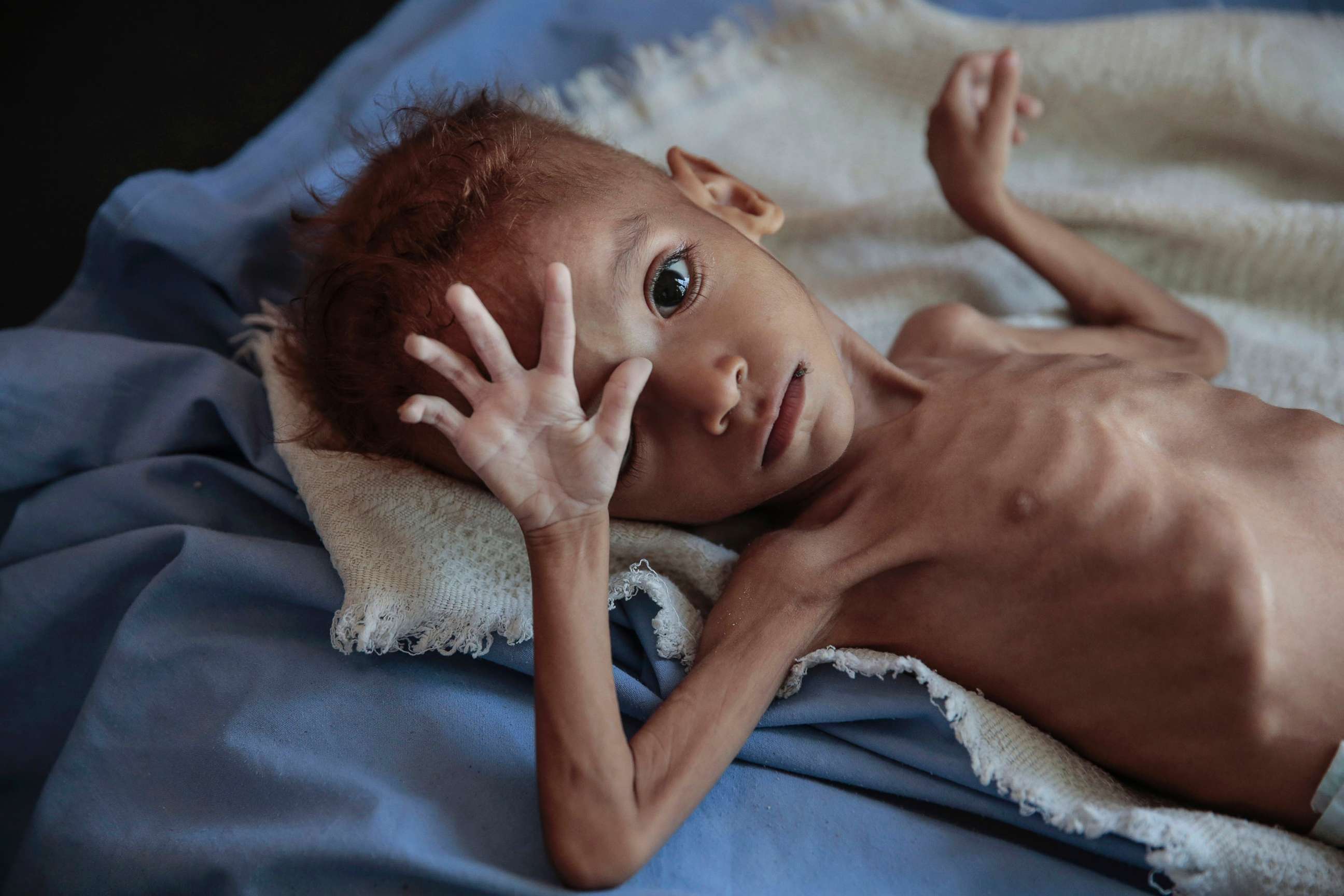
Starvation is a severe health issue caused by long-term lack of essential nutrients and energy. Treating this condition demands a thorough and carefully supervised method because the body’s functions are greatly impaired, and sudden refeeding can lead to significant health dangers. Whether it emerges during humanitarian emergencies, persistent neglect, or extreme eating disorders, managing starvation includes more than just replenishing nutrients; it also involves stabilizing various organ systems, preventing complications, and tackling root causes.
When the body is deprived of food over an extended period, it enters a catabolic state in which fat stores, muscle tissue, and internal organs are broken down to supply energy. This leads to significant weight loss, weakness, and the disruption of metabolic, hormonal, and immune functions. Electrolyte imbalances—especially low levels of phosphate, potassium, and magnesium—are common and can result in life-threatening complications such as cardiac arrhythmias and respiratory failure.
Since the body adjusts to a lack of food by reducing various functions, any abrupt rise in food consumption can be hazardous. This condition is referred to as refeeding syndrome, a potentially deadly alteration in fluids and electrolytes that might happen when nutrients are reintroduced too quickly.
The initial phase in addressing starvation involves conducting a comprehensive evaluation of the patient’s condition. Healthcare professionals assess vital signs, weight, body mass index (BMI), hydration status, and lab values, such as glucose, electrolytes, and the functioning of the kidneys and liver. Often, intravenous fluids are provided initially to resolve dehydration and correct electrolyte imbalances prior to the introduction of solid foods or nutritional formulas.
During this stabilization phase, it’s essential to monitor for signs of infection, cardiac instability, or neurological symptoms. Individuals who have been severely malnourished often exhibit bradycardia (slow heart rate), hypotension, and hypothermia, all of which need to be corrected cautiously to avoid shock or organ failure.
After a patient is stabilized, the gradual reinitiation of calorie intake starts slowly. Nutrition is commonly given through specialized oral supplements or nasogastric feeding if the patient cannot consume food. The initial caloric intake is deliberately kept low—typically ranging from 10 to 20 kilocalories per kilogram of body weight per day—and is increased incrementally over several days or weeks.
The nutritional profile is meticulously crafted. At first, carbohydrates are restricted to minimize the likelihood of refeeding syndrome. Simultaneously, proteins, fats, and vital micronutrients such as thiamine and B vitamins are provided to aid in metabolic recovery. Electrolytes like phosphate, potassium, and magnesium are replenished based on necessity and carefully observed during the entire procedure.
In certain situations, intravenous feeding, also known as parenteral nutrition, might be necessary, particularly when the gastrointestinal system is not functioning well. Nevertheless, this method is applied with care and generally as a final option because of potential complications.
In situations where hunger is associated with mental health issues, like anorexia nervosa or major depression, psychological assistance is crucial for healing. Treatment plans usually incorporate behavioral therapy, counseling, and psychiatric services to aid individuals in tackling skewed perceptions concerning food, self-image, or past trauma.
Likewise, social actions are essential in cases of poverty, neglect, displacement, or conflict. Humanitarian groups and medical teams frequently collaborate to offer both nutritional assistance and access to housing, fresh water, sanitation facilities, and resources for long-term rehabilitation. Educational programs on balanced diets and sustainable food practices are often integrated into community-driven initiatives.
Children suffering from starvation are particularly vulnerable due to their increased nutritional needs and developing bodies. Pediatric treatment protocols often rely on ready-to-use therapeutic foods (RUTFs), which are energy-dense, micronutrient-fortified pastes that do not require refrigeration or clean water for preparation.
Those nutritional therapies, like ones derived from peanut paste and milk powder, enable caregivers to provide care at home following initial stabilization within a medical environment. Severe acute malnutrition in children is commonly diagnosed through low weight-for-height ratios, noticeable wasting, or mid-upper arm circumference (MUAC), and treatment is customized based on these criteria.
Vaccination, deworming, and infection control are often included in pediatric protocols, as malnourished children are highly susceptible to diseases like measles, pneumonia, and diarrhea, which can quickly become fatal without intervention.
Full recovery from starvation does not end once weight is regained. Rehabilitative care often includes ongoing nutritional support, physical therapy to rebuild muscle mass and function, and regular health monitoring to detect lingering deficiencies or complications. In many cases, digestive issues, anemia, bone density loss, or psychological symptoms can persist long after visible signs of malnutrition are resolved.
Continuous follow-up is particularly vital in environments where the availability of food is inconsistent. In such circumstances, preventive measures—including food stability initiatives, support for agriculture, and education on maternal nutrition—are crucial in disrupting the pattern of malnutrition.
In humanitarian emergencies, such as natural disasters, armed conflict, or mass displacement, rapid response protocols for starvation are essential. Organizations like UNICEF, the World Food Programme (WFP), and Médecins Sans Frontières (Doctors Without Borders) deploy standardized treatment kits and mobile clinics to reach affected populations.
Emergency feeding centers are established to triage and treat children and adults with moderate to severe acute malnutrition. These centers often operate alongside broader relief efforts that address sanitation, shelter, and disease control, recognizing that malnutrition rarely exists in isolation.
Once the immediate health emergency is addressed, avoiding a relapse into hunger necessitates addressing the underlying issues. These could be poverty, lack of food security, social exclusion, or widespread disturbances caused by conflict or environmental changes. Comprehensive solutions typically comprise a mix of healthcare initiatives, economic growth strategies, and social support aimed at fostering strong communities.
In individual cases, nutrition education, regular medical check-ups, and support from social workers or community health teams can help reinforce healthy behaviors and detect early signs of relapse.
Addressing starvation encompasses more than just supplying nourishment. It necessitates a comprehensive, research-informed strategy that considers the body’s delicate condition, the mental effects of extended lack of nutrition, and the societal factors that initially contributed to malnutrition. Through meticulous preparation, healthcare supervision, and ongoing assistance, those impacted by starvation can recuperate and restore both their well-being and self-respect.